- What We Do
- Agriculture and Food Security
- Democracy, Human Rights and Governance
- Economic Growth and Trade
- Education
- Ending Extreme Poverty
- Environment and Global Climate Change
- Gender Equality and Women's Empowerment
- Global Health
- Water and Sanitation
- Working in Crises and Conflict
- U.S. Global Development Lab

Margaret M. McCluskey, RN, MPH
Senior Technical Advisor, HIV Vaccines
Margaret McCluskey is the senior technical advisor for HIV vaccines in the U.S. Agency for International Development (USAID) Office of HIV & AIDS (OHA) and has been a registered nurse since 1980, working on the HIV/AIDS epidemic in one capacity or another from the beginning.
Recent Blog Posts
- Welcome to the HIV and AIDS Research Blog
Benny Kottiri – May 18, 2016
“Are you still a nurse?”
It’s a funny question – one that I get all too often – working here at USAID in the Office of HIV & AIDS. It may be that my fellow clinicians at the Agency also field this inquiry and find it equally as curious, even slightly annoying. I usually respond with a simple, “Yes. And I always will be.”
The responses that run through my head, and heart, are a bit more colorful, and it seems fitting to share these as we, once again, mark May 18 as National HIV Vaccine Awareness Day.
Since 1997, when President Clinton called for urgent efforts toward a vaccine to prevent HIV infection and AIDS, this day has been an annual observance to recognize and thank the thousands of volunteers, community members, health professionals, and scientists who work together to find a safe and effective HIV vaccine.
So, how does one chase this vaccine and stay true to being a bona fide (and still licensed) registered nurse? The connections between being in a hospital caring for the sick and being in a vast bureaucracy trying to solve global health problems are actually easy to make.
As a nurse at a bedside, you take on the responsibility and privilege of caring for a sick person. You have the mandate to assist in the diagnosis of your patient’s illness and to do all you can to alleviate their suffering. This is laudable work to be sure! But one can take well-honed clinical skills and a commitment to deep caring and go beyond the bedside – through research – in hopes of exponentially multiplying the good that can be done. Specifically, in my case: by searching for a solution that may prevent droves of people from suffering the many ill-effects of the HIV/AIDS epidemic.
So, when I came to USAID 10 years ago, I simply shifted from the bedside of an individual patient to that of a global epidemic; to assist in the discovery of the one tool believed capable of thwarting HIV once and for all: A vaccine that can prevent HIV.
As OHA’s senior technical advisor for HIV Vaccine Research, I may not take a blood pressure or dole out pills every day, but my fingers are on the pulse of this nasty epidemic all day long, trusting that I am part of stopping the ridiculous misery it still continues to wield worldwide.
Due to the promise of a safe and effective HIV vaccine to dramatically change the course of the HIV/AIDS global epidemic, USAID has supported the search for this tool since 2001. In addition to the global good that will result from the introduction of an HIV vaccine by reducing new infections, the cost savings will be tremendous.
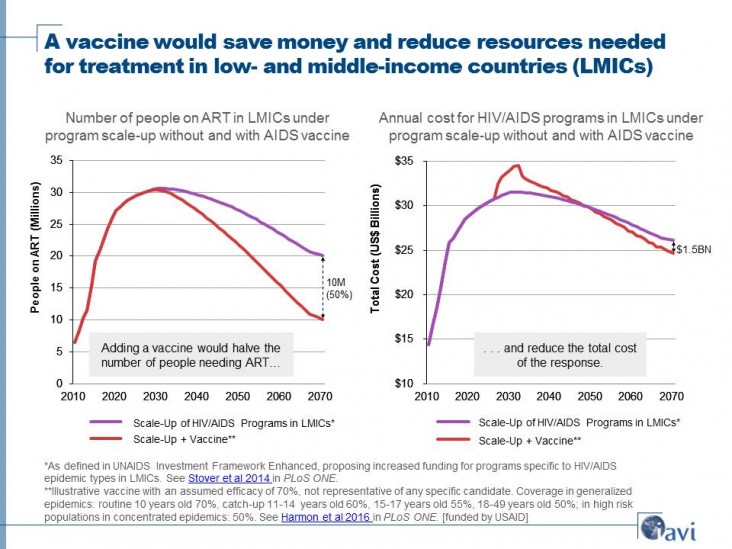
In an exercise by USAID’s long-time partner, the International AIDS Vaccine Initiative, the argument was made that even a 70 percent-effective HIV vaccine would translate into vast savings. The accompanying graphic provides a possible scenario in which an effective, well-implemented HIV vaccine would save serious resources by reducing the number of people requiring treatment as new infections are averted.
So, instead of ending long shifts in the hospital with laborious charting of the care given to each patient on my watch, I spend considerable time voraciously reading to keep current on the amazing science that will lead us to this elusive vaccine. I also provide in-depth technical concurrence to help my boss approve requests for important subawards to fund promising research; build bridges between partners, scientists, clinicians, donors, and community stakeholders; write new funding opportunities, etc. – and all of this is accomplished with a small but fabulous team in OHA’s Research Division.
The satisfaction I receive from doing my job in OHA is different than the comfort of throwing my lab coat on and wrapping my stethoscope across my neck every morning (which I still sorely miss). Yet, like caring for the sick, attending to this epidemic by guiding USAID investments toward the definitive tool to stop this tiny, but powerfully destructive, virus is truly a great privilege. We need an HIV vaccine to put an end to AIDS, and on May 18, there will be many reminders of this fact.
Additional Resources
- Read the brief: Investing in the Future: The Role of Africa in the Search for an HIV Vaccine [PDF, 570KB]







Comments
Question about IAVI's simulation
I have a question about IAVI's simulation of adding a 70% effective AIDS vaccine to the global AIDS toolkit. The Y-axis of the left-hand graph in this article shows "People on ART (US$ Millions)." I'm not very familiar with the ART work, so I'm not sure if person-dollars is some unit that I don't know, but $10-30 Million seems a little low in terms of global AIDS budget. Perhaps they didn't mean to include the "US$" in this label?
The promise of an AIDS vaccine seems extremely valuable in terms of human cost and dollars, and I'd love to learn more. Any clarification on this graph would be appreciated!
Graph replacement
Sylvie, thanks very much for your question on the graph. We’ve replaced the graph (left) with a corrected one showing the number of people on ART in millions on the y-axis instead of dollar amounts as the previous graph incorrectly featured.
"once a nurse, always a nurse"
Informative text. We still have a beautiful art piece at Misericordia, done by Margaret, when she worked here.
Add new comment